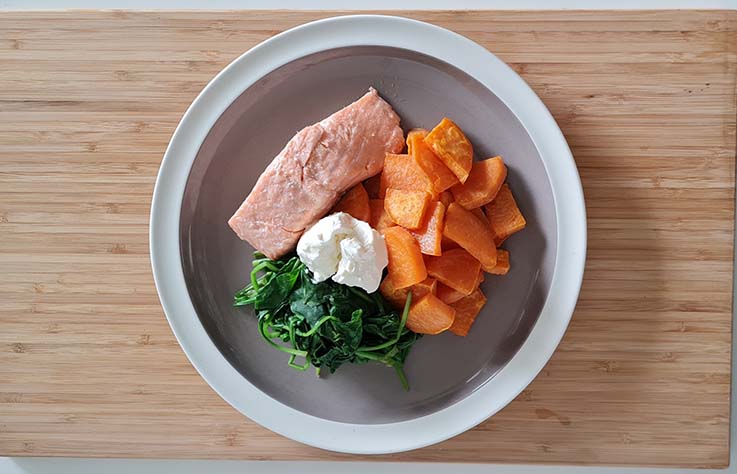Hanna & George's Tube Feeding Journey
Hanna describes her son George’s experience with tube feeding; from thinking it meant the end of oral feeding to learning it was actually the beginning.
Disclaimer: This article represents Hanna & George’s journey. Everyone’s tube feeding journey and nutritional needs are unique, so it’s important to speak with your enteral feeding dietician and/or healthcare professional before making any changes to a child’s feeding regimen.

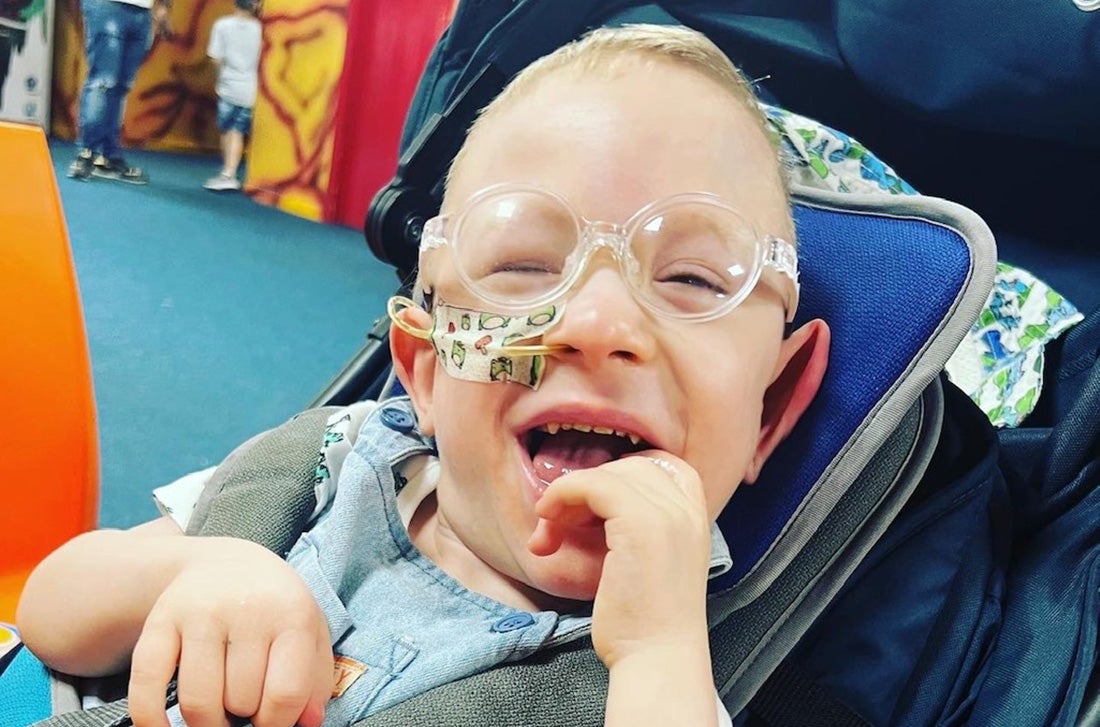
Meet George
Age: 3
Feed via: NG tube and orally
Fun fact: George can play with his spinning drum for 10 + hours a day and never get
bored!
George currently has a nasogastric (NG) tube fitted to support his oral feeding. He initially had the tube placed as he developed an aversion to food, so his healthcare professional suggested feeding via NG to ensure he was still meeting his daily nutritional requirements. Previous trial and error showed us that George was unable to tolerate any formula or prescribed tube feeds, as George was unable to keep them down and would projectile vomit almost straight after he was fed, but he was able to settle with real food. After some research and discussions with our medical team, it was decided that we would feed George a blended diet via his NG tube. It’s unusual for children with an NG tube to be fed a blended diet, due to the small size of the tube, but after much discussion with our Dietitian, it was the solution we decided on with their support. Once doing so George tolerated the new feeding regime and was able to have some of his medicines reviewed and stopped following guidance from our GP. Sickness and reflux no longer took over our lives.
Progress:
We were unsuccessful in getting any professional support when it came to tackling George’s food aversions due to the area we live in. We were told our therapists were not commissioned to help, and no out of area hospitals would accept us, which was very disappointing, but we did not give up.
Every single day George would be offered breakfast, lunch and dinner but for months he would only look at it and be fed via his tube. After a while, George started to take small bites before getting into the swing of things and beginning to enjoy food again. It was a very long and slow process but something we added into our everyday routine. George will now eat almost anything as long as it is the correct consistency, he loves a Sunday roast and chocolate yogurts!
Whilst we have the tube placed, we are able to take all pressure away from oral feeding and just go with what we could manage. Since then, George has started to enjoy food again and is now fully orally fed. George now only uses his tube for fluids, which we are in the process of weaning off too! It has been a long hard process, but the tube made it possible.
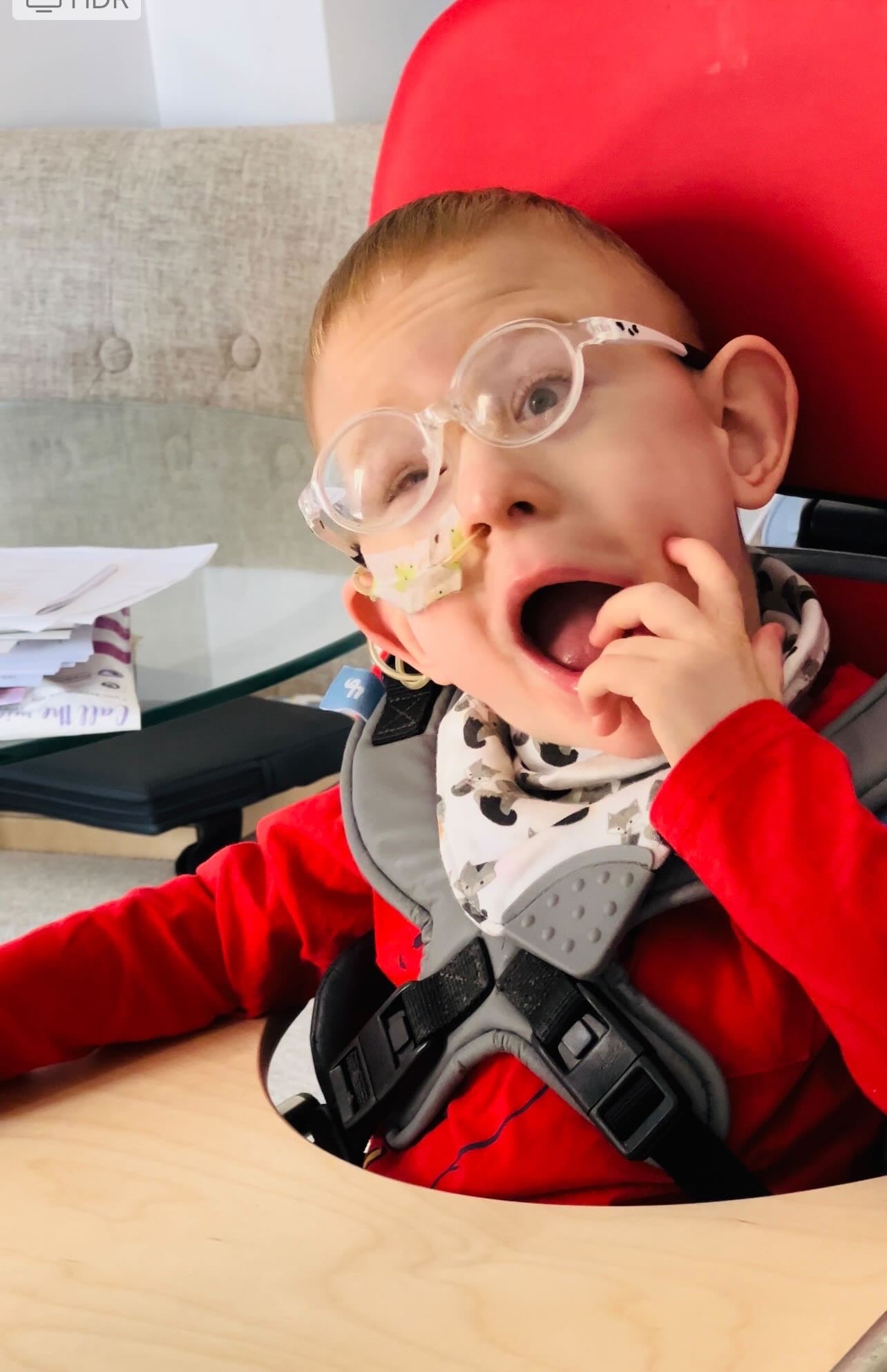
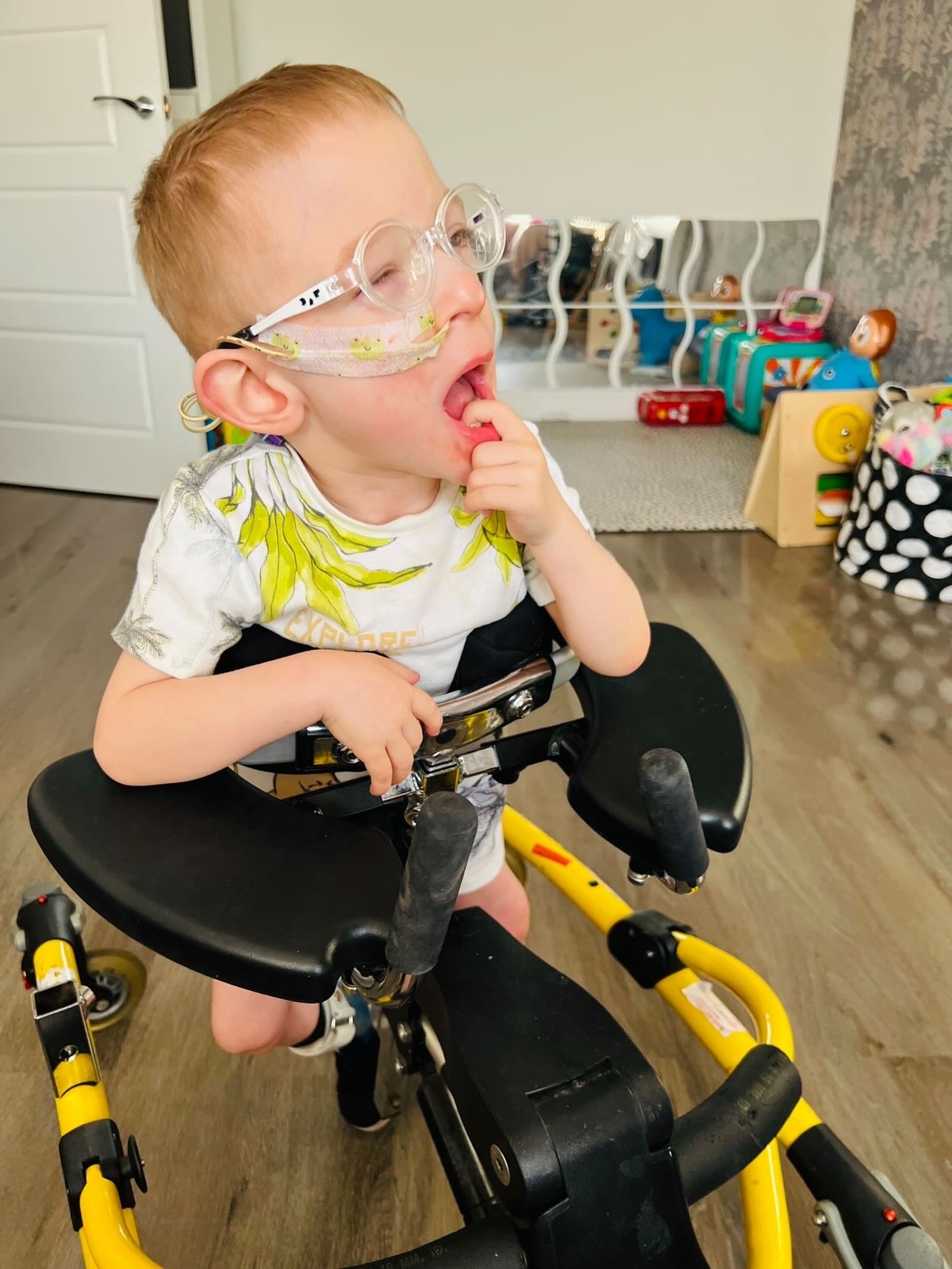
Our biggest struggle:
Our biggest struggle on our journey was the size of the nasal gastric tube. It’s so narrow that food would have to be watered down a lot to pass down the tube. As George was unable to tolerate high volumes, we needed to come up with low volume high calorie feeds. However, as George was extremely sensitive, these could also not be too rich. We eventually figured out that a plant-based, natural diet worked best for George. When professionals were able to see the progress George was making once we got the right balance, they were able to support our decision, which lifted a huge weight off my shoulders as a parent because I felt we could finally work as a team to give George what he needs.
When we were told George needed a nasogastric tube placed it was upsetting, and as a family we thought that was the end of Georges oral feeding journey, little did we know it was just the beginning.
If you would like to share your tube feeding stories or comments with us, we would love to hear from you, please email us on talkingtubefeeding@uk.nestle.com.
Make sure to check out more tube feeding stories from other tube feeding families, next. These articles are full of wisdom and hope!